Cancer of the Testes
Testicular Cancer is almost always curable if it is found early
It is the most common cancer in men between 15 – 35, but can strike any male any time!
Cancer of the testes is the most common cancer of men between 20 and 40, but it is in fact a rare cancer representing just 1% of cancer cases in men. It usually presents as a hard lump in the testes, which is usually painless. It is highly curable in its early stages. Depending on the stage at which it is diagnosed surgery alone can be used to treat it, or it may need to be treated with radiotherapy and or chemotherapy as well.
What is testicular cancer?
Cancer is an unregulated growth of cells. The testes are made up of two types of cells. One type of cell makes sperm; these are called the germ cells. The second type of cells in the testes support the germ cells. Testicular cancer is almost always an excessive growth of the germ cells. Cancers of the supporting cells are called stromal cancers and are very rare, and will not be discussed further.
Germ cell cancers can be divided into two basic types based on the cells found in the cancer, seminomas and non-seminomas (NSGCT). The two types of germ cell tumours are treated slightly differently. Seminomas grow more slowly and spread later, cure rates for early seminomas are of the order of 95%. NSGCT grow quicker, spread earlier and have a slightly lower cure rate but for early NGSCT this is still better than 90%. If the tumour is a mixture of seminoma and nonseminoma then it is treated as a nonseminoma (NSGCT).
What causes it?
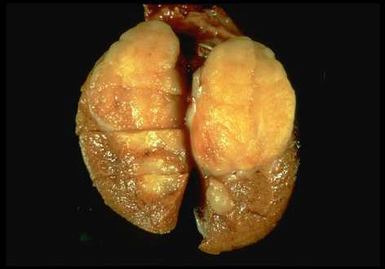
There is generally no cause found for testicular cancers. But the risk of developing testicular cancer is increased if you have had a testicle that did not come down into the scrotum (undescended testes), or one that was late to be put into the scrotum (maldescended). There can be a slightly increased risk if a brother or father had cancer of the testes. Testicular cancer is more common in white males and is also becoming more common over time, the reason for this is not known.
What tests do I need?
Almost always you will have had an ultrasound of the scrotum. This is to look at the lump in the testes and to check the other side. Once a cancer has been diagnosed the next step is to see whether there has been any spread. This is done with a CT scan of the abdomen and chest. Cancer of the testes spreads to the lymph nodes near the kidneys first and from there to the lymph nodes in the chest. Spread to other places such as the liver or bones is rare. You will often have an ultrasound of the testes as well.
Blood tests are also performed. Testicular cancers can make hormones that are picked up in blood tests. Seminomas make alpha-fetoprotein while non-seminomas can make both alpha-fetoprotein and beta HCG. These are chemicals that the foetus and or placenta normally make. In some ways they are useful to have, as they should go to normal values once the cancer is removed and therefore makes it easier to follow-up treatment.
How is it treated?
The first thing that is done is to remove the abnormal testicle. The testes and its sac and cord are removed by an operation. This is called a radical orchiectomy. The operation is done through a cut in the groin, much like the cut used to repair an inguinal hernia. Very rarely, if the cancer is very small just a piece is taken out of the testes instead.
Because testes cancer spreads along very well-defined lymphatic pathways the surgery is done through the groin with all layers surrounding the testes and it’s blood supply taken out intact with it intact. This is to minimise the chance of spreading the cancer to other parts of the body, which would not necessarily be treated or watched during follow-up.
Following surgery the testes is looked at by a pathologist to see what type of testicular cancer is present. Depending on the type of cancer and whether there is any evidence of spread to the lymph nodes you may be offered one of three choices
- Surveillance
- Radiotherapy
- Chemotherapy.
I have a seminoma what will happen?
If the cancer is a seminoma and there is no evidence of spread then you will be offered radiotherapy or two cycles of chemotherapy. If there is evidence of lymph node spread then you will be offered three cycles of chemotherapy. As Seminoma is very responsive to low-toxicity chemotherapy, often is blood test (tumour marker) negative it is rare to be offered surveillance.
I have a non-seminoma what will happen after surgery?
If the cancer is a nonseminoma then the treatment depends on
- The type of cancer (yolk sac, embryonal, teratoma)
- The blood test results (did you have an elevated blood test before and now it is negative)
- Is there any evidence of spread
- Are you reliable enough and keen enough for regular follow-up x-rays.
Depending on these factors you will be offered surveillance with regular CT scans or chemotherapy.
Will having my testicle removed affect my ability to have sex or being male?
No, You only need about half of one testicle to make enough testosterone to feel male and to have erections. You need about ¾ of testes to be fertile.
Will surgery affect my ability to have children later?
No, but for reasons that are unclear men who have had testes cancer have a lower fertility rate than men who have not. It is not clear if this is because of
Some inherent factor in the testicles that led to the cancer in the first place or if this is related to some aspect of treatment. In general if you have chemotherapy you should not try for a baby for one year after chemotherapy finishes. It may be a good idea to store sperm at fertility associates before treatment begins. No one knows if the best time to do this is before surgery or after it.
What does chemotherapy involve?
For early stage disease chemotherapy is very well tolerated. For Testicular seminoma two cycles of low toxicity drugs are given over about 2 months. For NSGCT this is usually extended to three cycles.
If the cancer has spread to the lymph nodes then a three-drug regime is usually given over many months. This can cause more side effects and this should be discussed with your oncologist.
What does radiotherapy involve?
Radiotherapy is used to treat people who have had a seminoma removed. Radiotherapy involves passing radiation through the lymph nodes where the cancer might have spread to. The dose used for testicular cancer is low as testicular cancer, especially seminomas, are very sensitive to radiotherapy. The dose is divided up into several small doses over two weeks, typically Monday to Friday.
You can keep working during the treatment and in general most patients tolerate the therapy very well. Side effects are typically a little bit of tiredness. Radiotherapy can however have some long-term late effects. As most men with testes cancer are young and are cured by therapy there has been a slight shift away from radiotherapy to chemotherapy to reduce the chances of late harm.
What happens if the cancer comes back?
If the cancer comes back then it usually comes back in the lymph nodes. This will mean chemotherapy. The chance of chemotherapy working is very high. Sometimes after the chemotherapy is finished there will be a lump left in the lymph node. This is then removed by surgery. This operation is called a retroperitoneal lymph node dissection. Very rarely bone marrow transplants are used if the cancer needs a lot of chemotherapy to eradicate it.
Where can I find further information?
Websites:
http://www.testicularcancersociety.org
Information:
http://www.macmillan.org.uk/Cancerinformation/Cancertypes/Testes/Testicularcancer.aspx
